What is the sol layer of the mucociliary escalator

Henry Morales
Published Apr 12, 2026
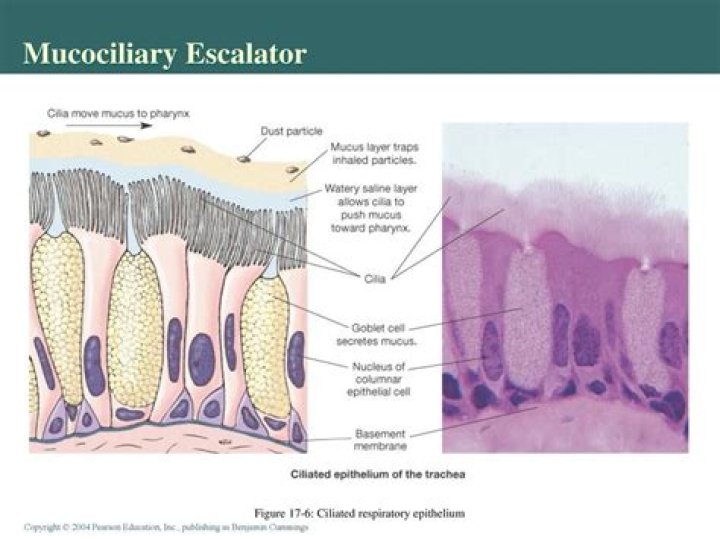
In the sol layer, also described as the ‘periciliary’ layer or ‘airway surface fluid’, the cilia beat and relax. The lubricant sol layer enables the gel mucus present at the tips of the cilia to be transported by the ciliary beating of the ciliated cells.
What is the sol layer?
It consists of 2 layers: (1) an inner serous layer (ie, sol phase) in which cilia recover from their active beat and (2) an outer, more viscous layer (ie, gel phase), which is transported by the ciliary beat.
What is the mucociliary escalator quizlet?
The layer of cleansing mucus moves upward to the pharynx from the lower portions of the bronchial tree on millions of hairlike cilia that cover the epithelial cells in the respiratory mucosa. The cilia beat or move only in an upward direction. This movement is sometimes called the mucociliary escalator.
What is the mucociliary escalator made up of?
The mucociliary escalator is inside of the conducting airways and is made up of mucus and cilia, which moves the mucus up and out of the lungs where it can be expelled by coughing or swallowing (Figures 1, 2) [5].What is mucociliary clearance and how does it work?
Mucociliary clearance is the primary mechanism to remove inhaled insoluble particles in the normal host. Inhaled particles that deposit in the ciliated airways are trapped in a blanket of mucus. This free-floating mucus gel overlies the respiratory epithelium.
What is mucociliary action?
Mucociliary clearance (MCC) is the primary innate defense mechanism of the lung. The functional components are the protective mucous layer, the airway surface liquid layer, and the cilia on the surface of ciliated cells.
What are the 2 parts of the mucociliary escalator?
The mucociliary escalator covers most of the bronchi, bronchioles and nose. It is composed of two basic parts: Mucous-producing goblet cells: The normal mucous film has two layers – the sol layer and the gel layer (Fig.
What is the function of the ciliary escalator?
of the Response of Lung to Air Pollutants The ciliary escalator transports mucus produced by mucous glands, goblet cells, and the Clara cells of bronchioles to the pharynx. Damage to cilia, changes in the volume and consistency of mucus, and in- jury to resriratory epithelial cells reduce mucus transport.How is the mucociliary escalator impaired in the intubated patient?
Mucociliary activity is impaired due to the presence of the artificial airway, airway trauma due to suctioning, inadequate humidification, high Fio2, drugs (eg, narcotics), and underlying pulmonary disease. Cough effectiveness is impaired due to the presence of the artificial airway and depressed neurologic status.
Which of the following best defines the mucociliary escalator?Which of the following best describes the mucociliary escalator? A. The mucociliary escalator sweeps away microbes and debris trapped in mucus. … The mucociliary escalator facilitates gas exchange in the alveoli.
Article first time published onWhich of the following best describes the mucociliary escalator group of answer choices?
Table 1. Overview of Nonspecific Innate Immune DefensesPhysical defensesMechanical defensesMicrobiomeChemical defensesChemicals and enzymes in body fluidsAntimicrobial peptides
What happens internal respiration?
Internal respiration occurs in the metabolizing tissues, where oxygen diffuses out of the blood and carbon dioxide diffuses out of the cells. In either case, diffusion occurs across the respiratory membrane from a high to a low partial pressure until equilibrium is achieved.
What is mucociliary clearance time?
Nasal mucociliary clearance times were less than 40 minutes in all the children. Normal children had nasal mucociliary clearance times of less than 24 minutes while significantly impaired nasal mucociliary clearance was detected in those with positive skin reactions and a positive response to methacholine challenge.
How does smoking damage the mucociliary escalator?
The upper regions of the bronchial tree are lined with ciliated cells, the “mucociliary escalator”, in charge of removing inhaled particles from the lungs. Chronic cigarette smoking may induce an increased number of abnormal cilia which could constitute a determinant of the mucociliary clearance impairment.
What is mucociliary blanket?
This “mucociliary blanket” serves to filter our air of tiny particles which can contain infection and other irritants which are then digested by acid in our stomach. The mucus contains defensive proteins that help protect us from invasion by organisms.
What is the mucociliary transport system?
Mucociliary transport. The term mucociliary transport or mucociliary clearance refers to a process in which coordinated waves of beating cilia move a blanket of mucus (and any material trapped within the mucus) progressively upward along the tracheobronchial tree.
What increases mucociliary drainage?
The rate of mucociliary clearance increases with greater hydration,2,73 and the rate of ciliary beating can be increased by purinergic, adrenergic, cholinergic, and adenosine-receptor agonists,60,73 as well as irritant chemicals. A second mechanism for the expulsion of mucus from the airways is cough clearance.
What does ciliary action accomplish?
These cilia have a rhythmic waving or beating motion. They work, for instance, to keep the airways clear of mucus and dirt, allowing us to breathe easily and without irritation. They also help propel sperm.
How can I improve my mucociliary escalator?
Heated, high-flow, humidified air or oxygen may improve mucus clearance by hydrating the mucus in the airways and may also help to increase airway patency. A similar intervention was shown to improve mucus clearance in subjects with bronchiectasis.
What is nasal mucociliary clearance?
The nasal mucociliary clearance system transports the mucus layer that covers the nasal epithelium towards the nasopharynx by ciliary beating. Its function is to protect the respiratory system from damage by inhaled substances. Impairment of nasal mucociliary clearance can result in diseases of the upper airways.
Which of the following are goals of airway clearance therapy?
The main goals of airway clearance techniques (ACTs) are to enhance mucus mobilization, reduce airway resistance, improve ventilation and gas exchange and to reduce work of breathing.
What is the function of the ciliary escalator quizlet?
The function of the “ciliary escalator” is to: a. remove microorganisms from the upper respiratory tract.
Which of the following describes the function of toll like receptors TLRs )?
Which statement best describes the role of Toll-like receptors (TLR) in the innate immune response? TLRs are found on leukocytes, or white blood cells. When a TLR is activated by the presence of its specific antigen, it stimulates and recruits various cells of the immune system.
What is the primary purpose of respiratory cilia quizlet?
Cilia line the nose and most other airways in the respiratory system. They trap dust and dirt particles and keep them from entering the lungs.
What are bronchioles?
Bronchioles are air passages inside the lungs that branch off like tree limbs from the bronchi—the two main air passages into which air flows from the trachea (windpipe) after being inhaled through the nose or mouth. The bronchioles deliver air to tiny sacs called alveoli where oxygen and carbon dioxide are exchanged.
Where does gas exchange occur?
During gas exchange oxygen moves from the lungs to the bloodstream. At the same time carbon dioxide passes from the blood to the lungs. This happens in the lungs between the alveoli and a network of tiny blood vessels called capillaries, which are located in the walls of the alveoli.
Where are the bronchial?
Your bronchi (BRAWN-kai) are the large tubes that connect to your trachea (windpipe) and direct the air you breathe to your right and left lungs. They are in your chest. Bronchi is the plural form of bronchus. The left bronchus carries air to your left lung.
Which of the following best describes the paroxysmal stage of pertussis?
The paroxysmal stage of Pertussis is characterized by episodes of coughing with a distinctive “whooping” sound when breathing in (inspiration). This characteristic cough gives the disease its common name, Whooping Cough. During the convalescent stage, episodes of coughing are less frequent and symptoms improve.
Which of the following anatomical structures is a part of the lower respiratory tract quizlet?
The upper respiratory tract includes the nose, mouth, nasal cavity, pharynx, and larynx. The lower respiratory tract consists of the trachea, bronchi, bronchioles, and lungs.
What is alveolar sac?
(al-VEE-oh-ly) Tiny air sacs at the end of the bronchioles (tiny branches of air tubes in the lungs). The alveoli are where the lungs and the blood exchange oxygen and carbon dioxide during the process of breathing in and breathing out.
What is the process of gas exchange in the alveoli called?
Diffusion is the spontaneous movement of gases, without the use of any energy or effort by the body, between the alveoli and the capillaries in the lungs.