What is a MTM plan

John Castro
Published Apr 05, 2026
Plans with Medicare drug coverage must offer free Medication Therapy Management (MTM) services if you meet certain requirements or are in a program to help members use their opioids safely. This program helps you and your doctor make sure that your medications are working to improve your health.
Who qualifies for MTM?
- You take eight or more Medicare Part D covered maintenance drugs.
- You have three or more of these long-term health conditions: Asthma. Chronic obstructive pulmonary disorder (COPD) Diabetes. Depression. …
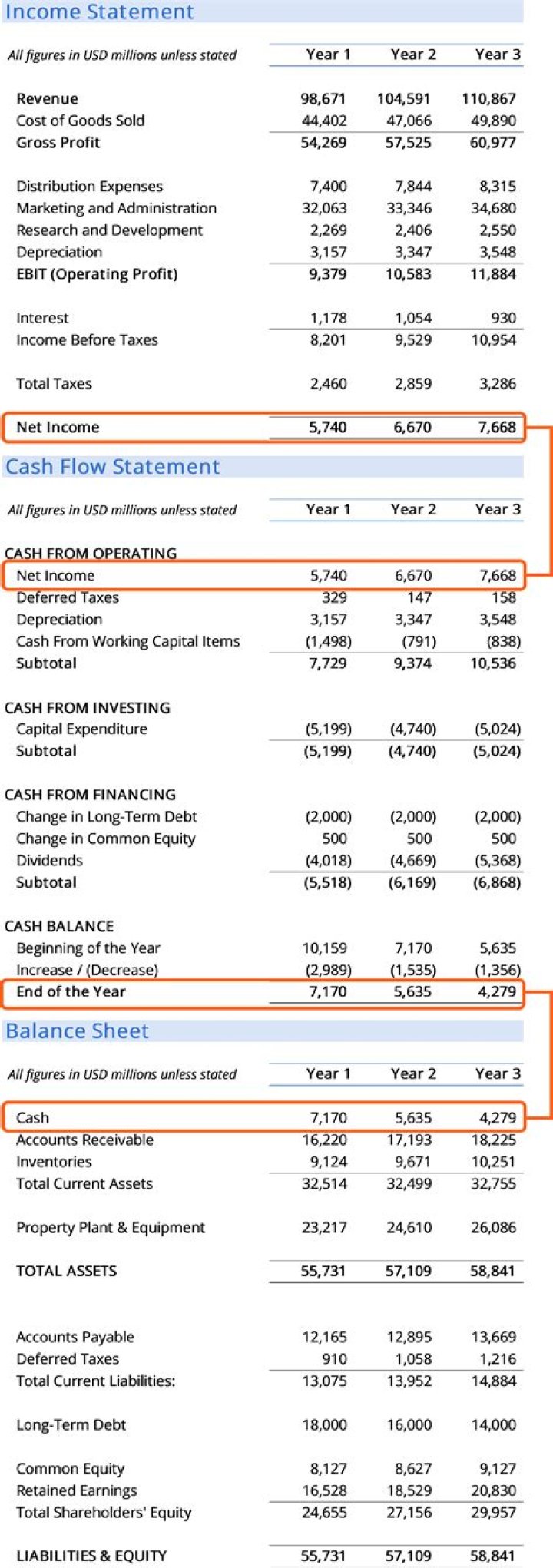
- You reach $4,376 in yearly prescription drug costs paid by you and the plan.
Who benefits from MTM services?
People who may benefit the most include those who use several medications, those who have several health conditions, those who have questions or problems with their medications, those who are taking medications that require close monitoring, those who have been hospitalized, and those who obtain their medications from …
Is MTM only for Medicare patients?
These services are free of charge to Medicare patients and eligibility is determined by their insurance plan. Non-Medicare patients who desire an MTM appointment can call the pharmacy to set up an appointment and expect to pay out-of-pocket.Who pays for MTM services?
º The patient is responsible for paying you in full for the MTM service provided at the time of the service.
How much does MTM services cost?
The 2019 MTM program annual cost threshold is $4,044, as compared to $3,967 in 2018.
What is the purpose of MTM?
The goal of MTM is to optimize the therapeutic outcomes of an individual patient as well as detect and prevent costly medication related adverse events.
What is the name of the legislation that required MTM services to be a part of Medicare Part D?
The Patient Protection and Affordable Care Act (PL 111-148) authorized grants for “medication management services” in all practice settings (Section 3503), noting that such services will help manage chronic disease, reduce medical errors, and improve patient adherence to therapies while reducing acute-care costs and …What is an MTM function that techs can perform in most states?
Technicians can provide support or management roles in MTM functions, such as the following: Medical and pharmacy record gathering, organization, and assessment. Medication reconciliation (developing a Personal Medication List) Correspondence with patients, physicians, other health care providers.
How does MTM benefit the patient?MTM has been shown to be effective for lowering systolic and diastolic blood pressure; lowering LDL cholesterol and other health indicators (e.g., glycosylated A1C, HbA1c); increasing patient knowledge; improving patient quality of life and medication adherence; and improving the safe and effective use of medications, …
Article first time published onWhat are the two critical aspects of MTM services?
There are two distinct components to medication management: medication reconciliation and medication review.
What is the difference between CMM and MTM?
In general, MTM may be regarded as more specific to the services applied for Medicare patients, while CMM is an approach used mainly in formalized collaborative practice settings such as accountable care organizations (ACOs).
Can a pharmacist bill for MTM?
MMA 2003 stated that: • Payers providing prescription drug benefits under Medicare Part D must establish MTM services for certain beneficiaries with chronic health conditions; • Providers can bill Medicare for performing MTM services; • Pharmacists are among the qualified professionals eligible to provide MTM services.
What are MTM CPT codes?
Three pharmacist-specific Current Procedural Terminology (CPT) codes exist to facilitate medication therapy management (MTM) reimbursement (codes 99605, 99606, and 99607). Large databases that contain these codes provide an opportunity to assess the effectiveness of MTM services.
Is medication therapy management mandatory?
You will be automatically enrolled in our Medication Therapy Management (MTM) program based on your specific medications and medical history. Participation is voluntary. You can opt out of the MTM program or any individual MTM service at any time by calling 1-888-686-4486 (TTY: 711).
How can you as a pharmacy technician recognize when a patient is a candidate for MTM?
Payers may review or “mine” patient utilization databases to identify those who are frequently hospitalized or seek emergency care may also target and identify patients who are candidates for MTM.
What do managed care pharmacists do?
Managing Quality and Cost Effectiveness of Medications Managed care pharmacists help health plans and other payers (e.g., employers, HMOs, trust funds, and Medicaid) evaluate and improve their pharmacy benefit by: Encouraging prescribers to make cost-effective drug choices that are clinically appropriate.
What do pharmacists do?
Pharmacists dispense prescription medications to patients and offer expertise in the safe use of prescriptions. They also may conduct health and wellness screenings, provide immunizations, oversee the medications given to patients, and provide advice on healthy lifestyles.
How long does it take to do a CMR?
A thoroughly executed CMR can take as long as 45 minutes to 1 hour. All medications and relevant medical conditions are evaluated. Action plans are developed, and patients are periodically reassessed. You should receive a CMR at least once a year.
Which item should patients bring to their MTM appointments?
Plan to bring the following items to your first MTM visit: Your health plan ID card and your Navitus ID card. A complete list of all of your medications (including dosage and frequency), or simply bring all of your prescription or over-the-counter medication bottles.
Which is the most correct order in which to don PPE when sterile compounding?
A. Gowning/garbing should take place in this order: placement of shoe covers, hair cover, face mask, proper hand washing technique, donning of gown, and finally the donning of sterile gloves.
What area does the non shedding gown cover?
Hence, the non-shedding gown (either disposable or launderable) should cover the full front of the individual up to the neck. For example, a gown that ties in the back should be used rather than one that buttons in the front. USP <797> does not expressly require that the gown provide full coverage in the back.
Is Medicare and Medicaid the same thing?
Medicare is a federal program that provides health coverage if you are 65+ or under 65 and have a disability, no matter your income. Medicaid is a state and federal program that provides health coverage if you have a very low income.
What is MTM CMR?
A key component of MTM is a CMR. A CMR is an interactive medication review or consultation between a patient and a pharmacist or other health care provid- er. In most cases it will take less than thirty minutes with the patient and may be completed over the phone, if permitted by the plan.
What is Medicare star?
The Medicare STARS program determines how well plans and providers perform across a section of quality measures using information from member satisfaction (both plan and providers), health outcomes and plan operations. A plan can get a rating from one to five stars. A 5-STAR rating is considered excellent.
When was MTM established?
BACKGROUND: In 2006, the Centers for Medicare & Medicaid Services (CMS) implemented the newly established Medicare Part D program that required plan sponsors to offer a medication therapy management (MTM) program.
What do you mean by drug therapy?
Drug therapy involves the administration of drugs to treat or prevent disease. It is used to treat a variety of illnesses and diseases ranging from psychiatric illnesses to the treatment of cancer. This type of therapy is also referred to as pharmacotherapy.
What is a prospective drug review?
1. Prospective DUR: Prospective review involves evaluating a patient’s planned drug therapy before a medication is dispensed. This process allows the pharmacist to identify and resolve problems before the patient has received the medication.
What is targeted medication review?
A targeted medication review (TMR) is an ongoing monitoring process with outreach made to the patient and/or prescriber about a specific or potential medication-related problem, without a comprehensive assessment of the patient’s medications.
Can Pharmacists Bill 99211?
For Medicare patients, pharmacists are not recognized as Medicare Part B providers and can only bill “incident-to” the physician supervising in the practice or clinic. Consequently, pharmacists are restricted to billing at the 99211 code level.
Does Medicare pay for 98960?
The CPT codes 98960, 98961 and 98962 are not separately billable services, and are either bundled into another service reported on the same day or are simply not covered. Do not report these codes to Medicare, unless required for secondary insurance.



