What do Kerley B lines look like

Henry Morales
Published Apr 15, 2026
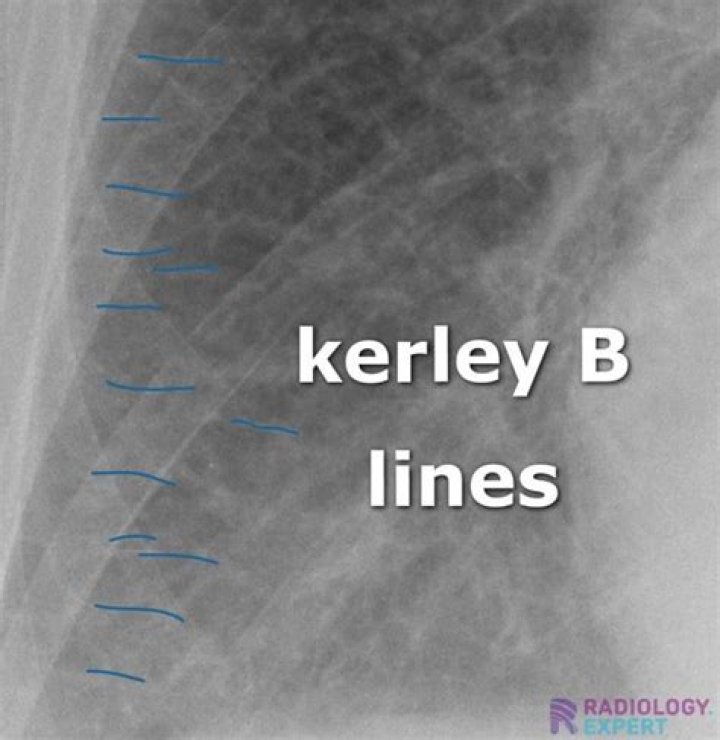
Kerley B lines (arrows) are horizontal lines in the lung periphery that extend to the pleural surface. They denote thickened, edematous interlobular septa often due to pulmonary edema.
How do I identify Kerley B lines?
Kerley B lines These are thin lines 1-2 cm in length in the periphery of the lung(s). They are perpendicular to the pleural surface and extend out to it. They represent thickened subpleural interlobular septa and are usually seen at the lung bases.
Are B lines normal?
Presence of multiple, diffuse, bilateral B-lines, associated to a normal heart, indicates a non-cardiac cause of pulmonary edema, as acute lung injury (ALI)/ARDS, interstitial pneumonia; alternatively, especially in a chronic setting, it should pose the suspicion of pulmonary fibrosis (Figure 5).
What does pulmonary edema look like on chest xray?
At chest radiography and CT, postobstructive pulmonary edema typically manifests as septal lines, peribronchial cuffing, and, in more severe cases, central alveolar edema (,Fig 10). These findings are similar to those in pressure edema.Is interstitial edema the same as pulmonary edema?
Florid pulmonary edema is frequently preceded by interstitial edema formation. Because of alterations in the balance of oncotic and hydrostatic pressures between the capillary and lung interstitium or changes in capillary permeability, edema fluid forms in the interstitial spaces of the lung.
What swollen lungs?
Pulmonary edema is a condition caused by excess fluid in the lungs. This fluid collects in the numerous air sacs in the lungs, making it difficult to breathe. In most cases, heart problems cause pulmonary edema.
What are Kerley B lines due to?
Causes of Kerley B lines include pulmonary edema, lymphangitis carcinomatosa and malignant lymphoma, viral and mycoplasmal pneumonia, interstitial pulmonary fibrosis, pneumoconiosis, and sarcoidosis. They can be an evanescent sign on the chest x-ray of a patient in and out of heart failure.
What do B lines represent?
B lines indicate filling of intralobular or interlobular septa and are often seen in pulmonary edema and interstitial lung diseases. Thickened B lines may fuse together to form coalescent B lines representing peripheral lung ground glass opacities seen in high resolution computed tomography (CT).How can you tell the difference between pulmonary edema and pneumonia?
The major difference being that pneumonia is an infectious pathology while pulmonary edema is not usually caused by an infection. It is a marker for a more severe underlying systemic pathology like heart failure or volume overload states in the body.
What do B lines mean?B lines, previously termed ”comet tails,” are vertical hyperechoic reverberations moving synchronously with the lung and represent key artifacts in interpreting pulmonary ultrasound findings [3,4]. The physiologic basis of B lines relates to decreased lung aeration [5], a finding that is nonspecific.
Article first time published onWhat are B lines in the lungs?
The B-line is a kind of comet-tail artifact indicating subpleural interstitial edema. The relationship between anterior interstitial edema detected by lung ultrasound and the pulmonary artery occlusion pressure (PAOP) value was investigated.
What is the life expectancy of someone with interstitial lung disease?
The average survival for people with this type is currently 3 to 5 years . It can be longer with certain medications and depending on its course. People with other types of interstitial lung disease, like sarcoidosis, can live much longer.
How serious is interstitial lung disease?
Interstitial lung disease can lead to a series of life-threatening complications, including: High blood pressure in your lungs (pulmonary hypertension). Unlike systemic high blood pressure, this condition affects only the arteries in your lungs.
What does interstitial fluid consist of?
Interstitial fluid contains glucose, salt, fatty acids and minerals such as calcium, magnesium and potassium. The nutrients in interstitial fluid come from blood capillaries Interstitial fluid can also hold waste products which result from metabolism.
What do damaged lungs feel like?
Coughing up blood: If you are coughing up blood, it may be coming from your lungs or upper respiratory tract. Wherever it’s coming from, it signals a health problem. Chronic chest pain: Unexplained chest pain that lasts for a month or more—especially if it gets worse when you breathe in or cough—also is a warning sign.
Can lungs hurt in your back?
Pleurisy, which is inflammation in the lining of the lungs, can cause sharp pains in the back and chest. This can often be the result of a viral or bacterial infection. Asthma, a chronic, long-term infection of the lung, may also cause pain in your back. Costochondritis is inflammation of rib cage cartilage.
What are the symptoms of a lung infection?
- Cough that produces thick mucus. Coughing helps to rid your body of the mucus produced from inflammation of the airways and lungs. …
- Stabbing chest pains. …
- Fever. …
- Body aches. …
- Runny nose. …
- Shortness of breath. …
- Fatigue. …
- Wheezing.
How can I remove fluid from my lungs at home?
- Steam therapy. Steam therapy, or steam inhalation, involves inhaling water vapor to open the airways and help the lungs drain mucus. …
- Controlled coughing. …
- Drain mucus from the lungs. …
- Exercise. …
- Green tea. …
- Anti-inflammatory foods. …
- Chest percussion.
What medications cause fluid in the lungs?
Additional drugs that can cause noncardiogenic pulmonary edema include carbamazepine, cytarabine, erythromycin, hydrochlorothiazide, IV radiographic contrast agents, methotrexate, protamine, tamoxifen, and tumor necrosis factor.
What are the 4 stages of pneumonia?
- Stage 1: Congestion. During the congestion phase, the lungs become very heavy and congested due to infectious fluid that has accumulated in the air sacs. …
- Stage 2: Red hepatization. …
- Stage 3: Gray hepatization. …
- Stage 4: Resolution.
How many B-lines are abnormal?
The presence of three or more B-lines per rib interspace in a longitudinal plane is abnormal and constitutes “B-pattern”.
What is lung point?
The interface of where healthy lung starts and where the pneumothorax ends is known as the lung point. On one side of the lung point, healthy pleura will be seen with pleural sliding, whereas on the other the pneumothorax will show a still pleural line with absent sliding.
What is alveolar interstitial syndrome?
Alveolar-interstitial syndrome was defined according to the Fleischner Society’s recommendations [16] as the presence of one or the combination of ground-glass opacities, consolidation, reticulation, and septal thickening.
What is the function of spirometer?
Spirometer. A spirometer is a diagnostic device that measures the amount of air you’re able to breathe in and out and the time it takes you to exhale completely after you take a deep breath. A spirometry test requires you to breathe into a tube attached to a machine called a spirometer.
What causes bline?
Causes of the interstitial syndrome include the following conditions (1): Pulmonary edema of various causes (including cardiogenic pulmonary edema and ARDS); Interstitial pneumonia or pneumonitis; Diffuse parenchymal lung disease (pulmonary fibrosis).
How many lines does the lungs have?
LungsThe human lungs flank the heart and great vessels in the chest cavityDetailsSystemRespiratory systemIdentifiers
What is lung point pneumothorax?
A typical lung point is sensitive and specific for pneumothorax. In the presence of a pneumothorax the visceral pleura falls away from the parietal pleura. The point at which the two pleural surfaces touch is called the lung point.
What are a lines ultrasound?
The A lines are horizontal artifactual repetitions of the pleural line displayed at regular intervals. The BLUE Protocol applies LUS and venous ultrasound for drawing profiles. A simplified echocardiography without Doppler can be associated with the BLUE protocol.
Do inhalers help interstitial lung disease?
Patients may be prescribed quick-relief and long-acting controller inhalers, as well as undergo oxygen therapy to improve lung function.
Can a person survive with scarred lungs?
There is no cure, and it eventually leads to death. Many things factor into how long and well people can live with pulmonary fibrosis. The disease may get worse quickly (over months) or very slowly (over years). Newer medications may help slow the disease progression.
Is interstitial lung disease a terminal illness?
Interstitial lung disease (ILD), especially idiopathic pulmonary fibrosis (IPF), is a fatal disease with a poor prognosis, and the therapeutic options are limited.