How many elements are common throughout all definitions of care coordination

Sarah Scott
Published Apr 17, 2026
Care coordination is described in a Commonwealth Fund report as one of seven elements needed to organize care around patients.
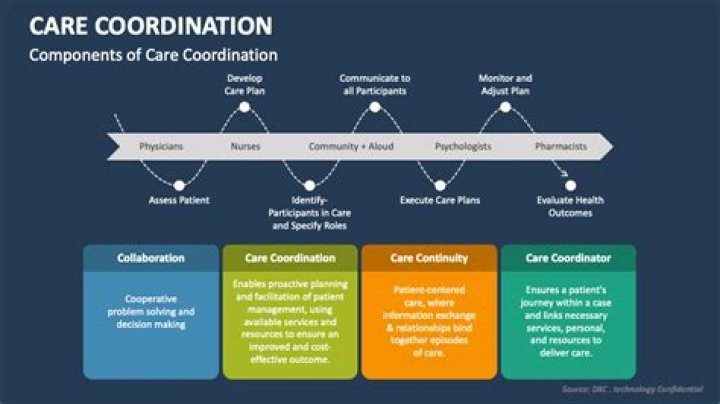
What are the components of care coordination?
- Establishing accountability and agreeing on responsibility.
- Communicating/sharing knowledge.
- Helping with transitions of care.
- Assessing patient needs and goals.
- Creating a proactive care plan.
What are the key attributes of care coordination?
Care coordination addresses potential gaps in meeting patients’ interrelated medical, social, developmental, behavioral, educational, informal support system, and financial needs in order to achieve optimal health, wellness, or end-of-life outcomes, according to patient preferences.
What is the definition of care coordination?
Based on their analysis, the researchers proposed a broad working definition of care coordination: “The deliberate organization of patient care activities between two or more participants (including the patient) involved in a patient’s care to facilitate the appropriate delivery of healthcare services.What is nurse care coordination?
The nurse care coordinator assists the patient by providing support and helping them navigate the medical system to get the care and treatment they need to prevent hospital readmission. An NCC is an RN who specializes in organizing patient care and treatments by including all members of the patient’s care team.
What is coordination and integration of care?
It is care that is planned with people who work together to understand the service user and their carer(s), puts them in control and coordinates and delivers services to achieve the best outcomes.
Whats a patient care coordinator?
A patient care coordinator, also known as a care coordinator, is the health professional who ensures that patients get the best care possible.
Which patients are often referred to care coordination programs?
Which patients are often referred to care coordination programs? Rationale: Patients with repetitive hospital readmissions are often referred to care coordination programs.What are the 3 levels of care?
- Primary Care.
- Secondary Care.
- Tertiary Care.
- Quaternary Care.
Care management, at its core, focuses on high-touch and episodic interactions; care coordination attempts to provide more longitudinal or holistic care.” Each of these tasks requires a slightly different set of stakeholders and its own unique health IT functionalities.
Article first time published onWhat is the importance of care coordination?
Care coordination has been identified as an important way to improve how the healthcare system works for patients, especially in terms of improved efficiency and safety. Most importantly, care coordination applied in a targeted way has the potential for improved outcomes for patients, providers, and payers.
What is the primary goal of care coordination quizlet?
What are goals of care coordination? What does care coordination allow? All health care/community services to work together so that patient and family needs can be met.
What are the seven elements that must be in place for a safe transition to occur?
Seven elements that must be in place for a safe transition to occur from one health setting to another include: leadership support; multidisciplinary collaboration; early identification of patients/clients at risk; transitional planning; medication management; patient and family action/engagement; and the transfer of …
How do I become a successful patient care coordinator?
- Provide easy access to a range of health care services and providers.
- Streamline all communications and care plan transitions between providers.
- Focus on the whole patient by addressing physical, emotional, social, mental, and financial needs.
What is care coordination in Nursing UK?
The care coordination service aims to keeps patients with complex health and care needs well at home. You can access this service if you: … Need help to find your way around different health and social care services.
How many integrated care systems are there?
ICSs (integrated care systems) are now seen by NHS leaders as the future of health and care integration in England. The NHS Long Term Plan and now the Government’s Health and Care Bill place ICSs at the heart of the NHS. As of April 2021, there are 42 ICSs covering every area in England.
What are the three strands of care available from the NHS?
NHS England’s Five Year Forward View described ways of breaking down the traditional divide between primary care, community services and hospitals.
What are the elements of primary health care?
- Education about prevailing health problems and how to prevent and control them.
- Food supply and proper nutrition.
- Adequate supply of safe water and basic sanitation.
- Maternal and child health, Family planning.
- Immunisation against infectious diseases.
- Prevention and control of endemic diseases.
What are the 4 main health care sectors?
These industries include pharmaceuticals, biotechnology, equipment, distribution, facilities, and managed health care.
What is level of care?
Assisted living “levels of care” generally refers to how much assistance a person needs with activities of daily living (ADLs) as well as management of one’s health. ADLs include tasks like getting dressed, taking a bath or shower, eating and using the restroom.
Who needs care coordination?
Coordination is necessary when participants are dependent upon each other to carry out disparate activities in a patient’s care; 3. In order to carry out these activities in a coordinated way, each participant needs adequate knowledge about their own and others’ roles, and available resources; 4.
What can you do with a MSN in care coordination?
- Patient/Nurse Advocate.
- Nurse Case Manager.
- Managed Care Nurse.
What is the definition of care management?
Care management is a promising team-based, patient-centered approach “designed to assist patients and their support systems in managing medical conditions more effectively.”3 It also encompasses those care coordination activities needed to help manage chronic illness.
What is the most common form of managed care?
The most common type of managed care plan is the HMO. If you enroll in an HMO plan, you’ll need to pick a primary care provider who will direct all your healthcare needs and refer you to specialists when appropriate.
Why is care coordination important in nursing?
Care coordination promotes greater quality, safety, and efficiency in care, resulting in improved healthcare outcomes and is consistent with nursing’s holistic, patient-centered framework of care.
Which method to improve coordination is used to arrange for and coordinate patient care?
Electronic health record (EHR) systems can decrease the fragmentation of care by improving care coordination. EHRs have the potential to integrate and organize patient health information and facilitate its instant distribution among all authorized providers involved in a patient’s care.
Who coordinates the implementation of the plan of care quizlet?
At 30 weeks gestation, the patient is ready for discharge. The nurse coordinates with the entire health care team to monitor and continually evaluate the effectiveness of the plan of care.
What is the first step in time management as a stress management tool?
Step 1: Write down your short-term and long-term goals. The key to time management is to know your goals, prioritize them and to focus on tasks and activities that help you reach those goals.
What is transitional care?
Transitional care encompasses a broad range of services and environments designed to promote the safe and timely passage of patients between levels of health care and across care settings. … These patients typically receive care from many providers and move frequently within health care settings.
What is transition in health and social care?
Transition is the purposeful planned movement of young adults with chronic conditions from child-centred to adult-orientated health care systems.
What is transitional care model?
The Transitional Care Model is designed to prevent health complications and rehospitalizations of chronically ill, elderly hospital patients by providing them with comprehensive discharge planning and home follow-up, coordinated by a master’s-level “Transitional Care Nurse” who is trained in the care of people with …