How is Hypophosphatemia diagnosed

William Harris
Published Apr 06, 2026
Hypophosphatemia is diagnosed by a serum phosphate concentration < 2.5 mg/dL (< 0.81 mmol/L). Most causes of hypophosphatemia (eg, diabetic ketoacidosis, burns, refeeding) are readily apparent.
How is hyperphosphatemia diagnosed?
Diagnosis is by serum phosphate measurement. Treatment includes restriction of phosphate intake and administration of phosphate-binding antacids, such as calcium carbonate. (See also Overview of Disorders of Phosphate Concentration. Most phosphorus in the body is complexed with oxygen as phosphate.
How are phosphate levels tested?
The phosphorus blood test measures the amount of phosphate in the blood. Blood is drawn from a vein (venipuncture), usually from the inside of the elbow or the back of the hand. A needle is inserted into the vein, and the blood is collected in an air-tight vial or a syringe.
How do you know if you have a phosphorus deficiency?
Symptoms of phosphorus deficiency include loss of appetite, anxiety, bone pain, fragile bones, stiff joints, fatigue, irregular breathing, irritability, numbness, weakness, and weight change. In children, decreased growth and poor bone and tooth development may occur.Which clinical manifestations are indications of hyperphosphatemia?
- muscle cramps or spasms.
- numbness and tingling around the mouth.
- bone and joint pain.
- weak bones.
- rash.
- itchy skin.
What causes phosphate levels to drop?
Hypophosphataemia is the term used to describe low levels of phosphate in the blood. It is most commonly caused by hyperparathyroidism and vitamin D deficiency.
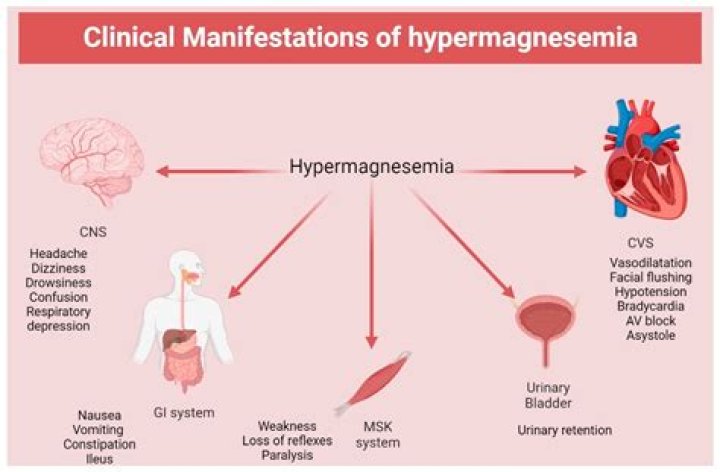
What are clinical manifestations hyperphosphatemia?
Signs and symptoms of acute hyperphosphatemia result from the effects of hypocalcemia, with patients occasionally reporting symptoms such as muscle cramps, tetany, and perioral numbness or tingling. Other symptoms include bone and joint pain, pruritus, and rash.
Why would phosphate levels be low?
If your phosphate levels are low, it may be a sign of: Alcoholism. Severe burns. Diabetic ketoacidosis (too much acid in the blood)What diseases cause low phosphorus?
- severe malnutrition, such as from anorexia or starvation.
- alcoholism.
- severe burns.
- a diabetes complication called diabetic ketoacidosis.
- the kidney disorder, Fanconi syndrome.
- an excess of parathyroid hormone (hyperparathyroidism)
- chronic diarrhea.
- vitamin D deficiency (in children)
A phosphate in blood test measures the amount of phosphate in your blood. Phosphate is an electrically charged particle that contains the mineral phosphorus. Phosphorus works together with the mineral calcium to build strong bones and teeth. Normally, the kidneys filter and remove excess phosphate from the blood.
Article first time published onWhat is the name of the blood test for phosphorus?
A phosphate test measures the amount of phosphate in a blood sample. Phosphate is a charged particle (ion) that contains the mineral phosphorus. The body needs phosphorus to build and repair bones and teeth, help nerves function, and make muscles contract.
What is phosphate in DNA?
A phosphate backbone is the portion of the DNA double helix that provides structural support to the molecule. DNA consists of two strands that wind around each other like a twisted ladder. Each strand has a backbone made of alternating sugar (deoxyribose) and phosphate groups.
What causes hyperphosphatemia in hypoparathyroidism?
Hypoparathyroidism causes hyperphosphatemia through a failure of the kidneys to inhibit renal proximal tubule phosphate reabsorption. Syndromes of tubular resistance to PTH manifest hyperphosphatemia because of the same mechanism.
What is considered severe hyperphosphatemia?
Severe hyperphosphatemia, defined herein as levels of 14 mg/dL or higher, is almost invariably multifactorial–usually resulting from addition of phosphorus to the extracellular fluid together with decreased phosphorus excretion.
Does hyperphosphatemia cause hypocalcemia?
The ensuing hyperphosphatemia may induce potentially symptomatic hypocalcemia due to calcium-phosphate precipitation in the tissues. Calcifications can also be present in skin, soft tissue, and periarticular regions. Prolonged bone demineralization can lead to bone fractures.
What are the symptoms of hypoparathyroidism?
- Tingling or burning in your fingertips, toes and lips.
- Muscle aches or cramps in your legs, feet, stomach or face.
- Twitching or spasms of your muscles, particularly around your mouth, but also in your hands, arms and throat.
- Fatigue or weakness.
- Painful menstrual periods.
What is a uremic patient?
Uremia is a dangerous condition that occurs when waste products associated with decreased kidney function build up in your blood. Uremia means “urine in the blood” and refers to the effects of the waste product accumulation. It affects the entire body.
Is hyperphosphatemia an emergency?
Advanced chronic kidney disease (GFR < 25 mL/min) is commonly associated with hyperphosphatemia. Such patients are particularly susceptible to developing severe and life-threatening hyperphosphatemia if they are exposed to an acute increase in serum phosphate levels.
What is the difference between hypophosphatasia and hypophosphatemia?
In hypophosphatasia, mineralization is disrupted affecting a number of tissues, including bone and teeth. With X-linked hypophosphatemia, an inability of the cells in the body to properly process phosphate causes circulating levels of phosphate to be low, resulting in problems with bone and tooth development.
What medications treat hypophosphatemia?
Drug nameRatingRx/OTCView information about Calciferol CalciferolRateRx/OTCGeneric name: ergocalciferol systemic Drug class: vitamins For consumers: dosage, interactions, side effectsView information about Calcidol CalcidolRateRx/OTC
How do you treat hypophosphatemia?
Treatment of hypophosphatemia is twofold: (1) correct any precipitating causes of hypophosphatemia, and (2) replace total body phosphates. Depending on the clinical situation, replacement options include dietary phosphate, oral phosphate preparations, and IV phosphate.
What is the most common cause of hypophosphatemia?
Hypophosphatemia is most often caused by long-term, relatively low phosphate intake in the setting of a sudden increase in intracellular phosphate requirements such as occurs with refeeding. Intestinal malabsorption can contribute to inadequate phosphate intake, especially if coupled with a poor diet.
How long does it take to recover from Hypophosphatemia?
In this group, serum phosphate levels decrease to a nadir within approximately 2 days and recover in the following days. This early nadir is also described after cardiac surgery and in patients with diabetic ketoacidosis and the refeeding syndrome.
Who is most at risk for a phosphorus deficiency?
Research shows that people who are overweight or obese are more likely to have inadequate intakes and low blood levels of certain vitamins and minerals compared to those who are at a normal weight ( 11 , 12 ).
Can Hypophosphatemia cause death?
Acute severe hypophosphatemia can cause serious neuromuscular disturbances, rhabdomyolysis, seizures, coma, and death.
What is severe hypophosphatemia?
Hypophosphatemia is defined as mild (2-2.5 mg/dL, or 0.65-0.81 mmol/L), moderate (1-2 mg/dL, or 0.32-0.65 mmol/L), or severe (< 1 mg/dL, or 0.32 mmol/L). Mild to moderately severe hypophosphatemia is usually asymptomatic.
What is the normal range of serum phosphate?
Adult: 3.0-4.5 mg/dL or 0.97-1.45 mmol/L (SI units) Elderly: values slightly lower than adult. Child: 4.5-6.5 mg/dL or 1.45-2.1 mmol/L (SI units) Newborn: 4.3-9.3 mg/dL or 1.4-3 mmol/L (SI units)
How will you detect the presence of phosphorus in an organic compound?
The organic compound is heated with an oxidising agent. The phosphorus present in the compound is oxidized to phosphate. The solution is boiled with nitric acid and then treated with ammonium molybdate . A yellow colouration indicated presence of phosphorus.
Is fasting required for phosphorus blood test?
What is the procedure for a serum phosphorus test? You don’t typically need to fast before this test. Your doctor will let you know if they want you to fast for any reason. The test involves a simple blood draw.
What are the 3 types of DNA?
Three major forms of DNA are double stranded and connected by interactions between complementary base pairs. These are terms A-form, B-form,and Z-form DNA.
What are the 4 bases of DNA?
There are four nucleotides, or bases, in DNA: adenine (A), cytosine (C), guanine (G), and thymine (T). These bases form specific pairs (A with T, and G with C).