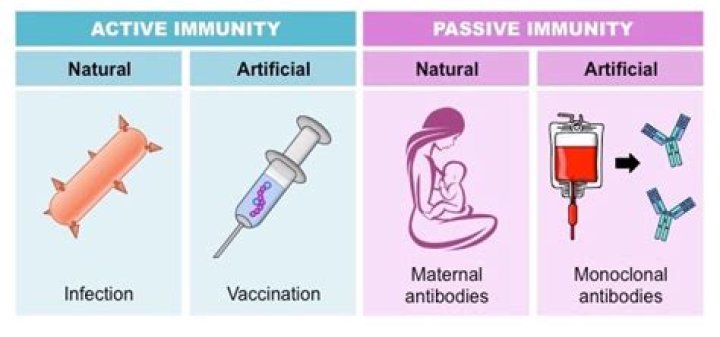
Can you get passive immunity from blood transfusions

Emily Cortez
Published Apr 17, 2026
If you were treated for COVID-19 symptoms with monoclonal antibodies or convalescent plasma, you should wait 90 days before getting a COVID-19 vaccine.
Can you get the COVID-19 vaccine if you were treated with antibodies or plasma?
If you were treated for COVID-19 symptoms with monoclonal antibodies or convalescent plasma, you should wait 90 days before getting a COVID-19 vaccine.
Who is not eligible for the COVID-19 vaccine?
Children younger than age 5 years are not eligible to receive the Pfizer-BioNTech COVID-19 Vaccine at this time unless part of a clinical trial. Children and adolescents younger than age 18 years are not eligible to receive the Moderna or Janssen COVID-19 vaccines at this time.
Would COVID-19 antibody test be positive after vaccine?
Be aware that if you have a positive test result on a SARS-CoV-2 antibody test, it is possible you were previously infected with SARS-CoV-2. A COVID-19 vaccination may also cause a positive antibody test result for some but not all antibody tests.What medication is not recommended before vaccinations for COVID-19?
It is not recommended you take over-the-counter medicine – such as ibuprofen, aspirin, or acetaminophen – before vaccination for the purpose of trying to prevent vaccine-related side effects. It is not known how these medications might affect how well the vaccine works.
Can I get the COVID-19 vaccine if I have an underlying condition?
People with underlying medical conditions can receive a COVID-19 vaccine as long as they have not had an immediate or severe allergic reaction to a COVID-19 vaccine or to any of the ingredients in the vaccine. Learn more about vaccination considerations for people with underlying medical conditions. Vaccination is an important consideration for adults of any age with certain underlying medical conditions because they are at increased risk for severe illness from COVID-19.
Should I get the COVID-19 vaccine if I have recovered from COVID-19?
If I have already had COVID-19 and recovered, do I still need to get vaccinated with a COVID-19 vaccine? Yes, you should be vaccinated regardless of whether you already had COVID-19 because: Research has not yet shown how long you are protected from getting COVID-19 again after you recover from COVID-19. Vaccination helps protect you even if you’ve already had COVID-19.
Should you get the Covid vaccine if you have an autoimmune disease?
The American College of Rheumatology COVID-19 Vaccine Clinical Guidance recommends that people with autoimmune and inflammatory rheumatic disease (which includes lupus) get the vaccine unless they have an allergy to an ingredient in the vaccine.Can taking immunosuppressants increase my chances of getting COVID-19?
And medicines called immunosuppressants may make you more likely to have serious complications from the virus, as can your autoimmune disorder itself
Do COVID-19 antibody tests detect vaccine antibodies?• Some antibody tests will only detect antibodies from infection, not from vaccination with the virus that causes COVID-19.
Article first time published onHow long after getting infected will COVID-19 antibodies show up in the test?
An antibody test may not show if you have a current infection because it can take 1–3 weeks after the infection for your body to make antibodies.
Can I get COVID-19 again?
In general, reinfection means a person was infected (got sick) once, recovered, and then later became infected again. Based on what we know from similar viruses, some reinfections are expected. We are still learning more about COVID-19.
Can I get reinfected with COVID-19 after I have been vaccinated in Kentucky?
These findings suggest that among persons with previous SARS-CoV-2 infection, full vaccination provides additional protection against reinfection. Among previously infected Kentucky residents, those who were not vaccinated were more than twice as likely to be reinfected compared with those with full vaccination.
Is having a heart condition considered as high risk for COVID-19?
Having heart conditions such as heart failure, coronary artery disease, cardiomyopathies, and possibly high blood pressure (hypertension) can make you more likely to get severely ill from COVID-19.
Can immunosuppressive drugs increase the risk of serious COVID-19 infection?
According to the study’s authors, drug-induced immunosuppression could potentially elevate the risk of severe COVID-19 symptoms and hospitalization if these individuals become infected. Data for the study was gathered from more than 3 million patients with private insurance.
Which groups of people are at increased risks of severe illness from COVID-19?
Among adults, the risk for severe illness from COVID-19 increases with age, with older adults at highest risk. Severe illness means that the person with COVID-19 may require hospitalization, intensive care, or a ventilator to help them breathe, or they may even die. People of any age with certain underlying medical conditions are also at increased risk for severe illness from SARS-CoV-2 infection.
Are rheumatoid arthritis patients more at risk of getting COVID-19?
If you have rheumatoid arthritis (RA), you’re more likely to get certain infections. That means you may have a higher chance of getting COVID-19. If you do get sick, your symptoms could be more serious than someone who doesn’t have RA. Some medicines you take might also make infections more likely.
Are you at risk of experiencing an autoimmune disease flare-up from COVID-19 vaccine?
There is a risk that flare-ups may occur. That being said, it has been observed that people living with autoimmune and inflammatory conditions are at higher risk of experiencing severe symptoms from a COVID-19 infection.
Would COVID-19 antibody test be positive after vaccine?
Be aware that if you have a positive test result on a SARS-CoV-2 antibody test, it is possible you were previously infected with SARS-CoV-2. A COVID-19 vaccination may also cause a positive antibody test result for some but not all antibody tests.
Why antibody testing Is not currently recommended to assess immunity after COVID-19 vaccination?
Currently authorized SARS-CoV-2 antibody tests have not been evaluated to assess the level of protection provided by an immune response to COVID-19 vaccination. If antibody test results are interpreted incorrectly, there is a potential risk that people may take fewer precautions against SARS-CoV-2 exposure.
Does an antibody test diagnose an active COVID-19?
Antibodies can take several days or weeks to develop after you have an infection and may stay in your blood for several weeks after recovery. Because of this, antibody tests should not be used to diagnose an active coronavirus infection.